Non-Surgical Herniated Disc Treatment Options Explained
April 22, 2026Hearing the words “herniated disc” often leads to an immediate fear of surgery. It can make the situation feel urgent, as if something in your spine has permanently gone wrong.
What’s usually lost in that moment is the fact that discs change over time. They respond to posture, age, and even small repetitive stresses. A herniation is not always a sudden failure. In many cases, it is a part of how the spine reacts to constant strain.
The pain is caused by the irritation around a nerve, not by the size of the disc bulge. A larger bulge doesn’t always mean more pain, and a smaller one does not always mean less. What’s important is how inflamed or sensitive the nerve has become.
So the next step is not automatically surgery. It is understanding what is driving your symptoms and how to manage them properly.
Understanding the Pressure on Your Spine
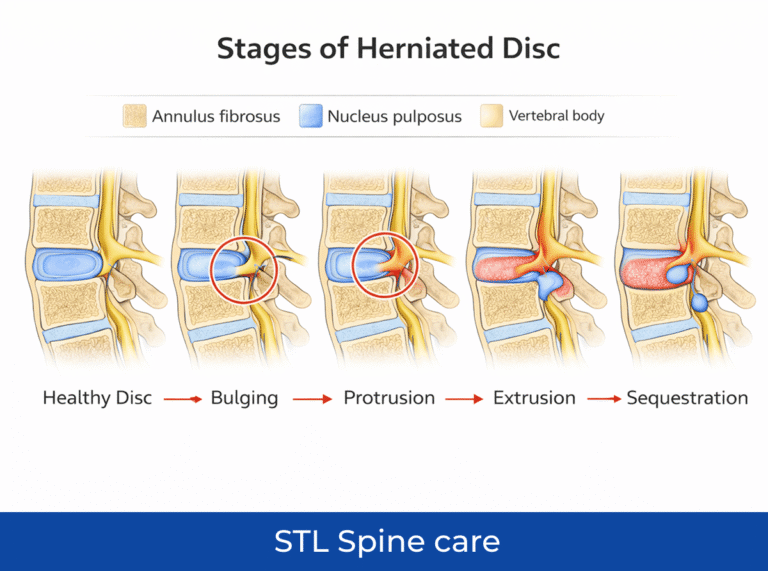
Think of your spinal discs as the “shock absorbers” of your body. They are tough on the outside, but filled with a soft center. A herniation happens when that soft layer pushes through a tear in the outer ring.
The pain you feel is not simply the disc pressing against a nerve. It is often the reaction that follows. When the inner material comes into contact with nearby tissues, it can trigger inflammation.
That inflammatory response makes the nerve more sensitive, which is why even small movements can suddenly feel sharp or intense.
When Is Surgery Not Needed?
Surgery fixes a structural problem, but most herniated disc pain comes from nerve irritation, not a permanent injury.
If you can still move your feet, control your bladder, and manage daily activities, non-surgical treatment is usually enough. Surgery is generally needed only when symptoms do not resolve with conservative care or if you lose important functions.
Ways to Relieve Herniated Disc Pain Without Surgery
Herniated disc pain relief is not about forcing the disc back into place. You feel pain because the nerves are reacting to irritation, and the body often knows how to heal itself.
It’s worth knowing that the discs in your lower back carry the most weight every day, which makes the lumbar region the most common spot for herniations. There are several ways to do this, each helping in its own way.
Physical Therapy
Physical therapy focuses on finding the exact movements that reduce your pain. A therapist may guide you through gentle extensions, slight tilts, or other directional exercises that shift discomfort away from your leg and back toward the spine, which usually means the disc is under less pressure and can induce the healing process.
Therapy also focuses on strengthening the muscles that support the spine, providing stability and reducing stress on the affected disc.
Minimally Invasive Interventions
When pain remains intense even after rest, medication, or early therapy, it often indicates that the nerve irritation has not resolved yet. In these situations, targeted procedures can be used to reduce inflammation in the affected area, so the nerve is not constantly reacting to the disc bulge.
| Treatment | How it Works | Best For |
|---|---|---|
| Epidural Steroid Injection (ESI) | Anti-inflammatory injection guided by X-ray | Severe leg pain (sciatica) |
| Nerve Blocks | Local anesthetic near the nerve root | Short-term pain relief or diagnosis |
| Radiofrequency Ablation | Heat is applied to nerves to block pain signals | Chronic face joint pain |
Activity Modification
Managing herniated disc pain doesn’t mean lying in bed. Prolonged rest actually weakens your core and stiffens the spine. Instead, small, strategic adjustments make a big difference.
Swap heavy lifting for smart lifting and implement the “20-minute rule”: never stay in one posture (sitting or standing) for more than 20 minutes. It keeps the disc hydrated and the blood flowing, which helps healing.
Spinal Decompression Therapy
Spinal decompression therapy gently stretches the spine using specialized equipment. Patients lie on a motorized table with pelvic harnesses while the device applies controlled pulls and releases, typically between 50–80 pounds over 20–45 minutes.
This treatment targets the lower lumbar discs, most commonly L4-L5 and L5-S1.
The gentle traction creates a small vacuum effect, relieving pressure on the disc, encouraging it to retract slightly, and drawing nutrient-rich fluid into dehydrated areas. Over time, this can reduce intradiscal pressure by up to 100 mmHg and help restore mobility while reducing pain.
Red Flags: When Your Body Needs Immediate Attention
While most herniated discs improve with non-surgical care, certain warning signs mean you should seek medical attention immediately:
- Sudden leg weakness – Difficulty walking, climbing stairs, or standing for long periods.
- Loss of bladder or bowel control – Any change in bathroom function can indicate serious nerve compression.
- Numbness in the saddle area – The region that would contact a saddle, this may signal serious nerve compression
- Foot drop – Trouble lifting the front part of your foot while walking.
- Rapidly worsening symptoms – Pain, tingling, or weakness that intensifies quickly and interferes with daily activities.
Recovering Without Surgery: How Your Body Heals a Herniated Disc
Many people are surprised to learn that herniated discs can shrink or even disappear on their own over time. Here’s how it happens:
- Resorption in action: Your immune system recognizes the leaked disc material as “out of place” and gradually breaks it down.
- Pressure relief: As the disc shrinks, nerves get more space, reducing irritation and pain.
- Visible results: In some cases, MRIs taken months later show the herniation has significantly decreased or even gone completely.
- Timeline: This natural repair process takes weeks to months, so patience and consistent care are important.
Conclusion
A herniated disc diagnosis doesn’t automatically put you on a surgical path. In many cases, it simply means your spine needs structured, conservative care and time to settle. By managing nerve irritation and guiding correctly, the body begins to improve on its own.
For patients who want clarity instead of urgency, working with experienced providers like STL Spine Care can help you explore non-surgical options thoughtfully and safely. With a thorough evaluation, patients gain clarity about their condition and can explore non-surgical treatment options first, without feeling pressured to undergo surgery.
Frequently Asked Questions
What is spinal decompression therapy, and how does it work?
It gently stretches the spine using specialized equipment, creating space for the disc to retract slightly and allowing nutrients to flow back into the injured area.
Are minimally invasive procedures safe for herniated disc pain?
When performed under professional guidance, procedures like epidural steroid injections or nerve blocks can safely reduce inflammation and pain, supporting other non-surgical treatments.
How long does it typically take to notice improvement with non-surgical care?
Improvement usually begins within a few weeks of consistent care. Full recovery can take several months, depending on the severity of the herniation and adherence to the recommended plan.
Can exercise make a herniated disc worse?
Certain movements may aggravate symptoms; therapist-guided exercises are designed to reduce nerve irritation and strengthen spinal support safely.
How does the body naturally reabsorb herniated disc material?
The immune system identifies leaked disc material as foreign and gradually breaks it down, relieving pressure on nerves and promoting recovery.
