Top 5 Signs That You May Have a Herniated Disc
April 2, 2026You bent over to tie your shoe, reached for a coffee mug, or maybe you just sneezed and, suddenly, you felt a sharp bolt of pain through your back.
Millions of people experience moments like this, but because lower back discomfort usually follows everyday lifestyle choices of a person, it can be easy to dismiss it as just a normal part of life.
While a pulled muscle usually fades with a few days of rest, a herniated disc is a different story; it’s a structural issue that puts your nerves under pressure. A herniated disc symptom can mimic a simple strain at first, but if left untreated, the condition can become serious. Here is how to tell if your discomfort is a simple ache or a disc that needs professional attention.
How to Know If You Have a Herniated Disc
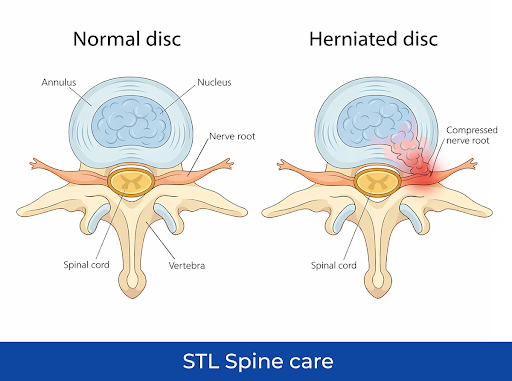
Think of a spinal disc like a jelly donut. The outer layer is tough and sturdy like the dough, while the inner portion is soft and squishy, like the jelly. When everything is fine, the disc cushions your spine and absorbs everyday movements without issue. But if the outer layer tears or weakens, the jelly-like inner material can push out.
When this “leak” presses on nearby nerves, it can trigger a variety of symptoms. Here are five key signs of a herniated disc that your back or neck pain may be more than a simple strain.
1. Pain That Radiates Down Your Leg or Arm
One of the clearest signs of nerve involvement is pain that travels along the path of the affected nerve.
In lumbar herniations, this often presents as sciatica, sharp or burning pain that shoots down the back of one leg. For cervical herniations, it can travel down the arm, sometimes accompanied by tingling or numbness in the fingers.
Unlike general muscle soreness, this pain doesn’t stay in one spot and often worsens with specific movements like bending, coughing, or sneezing.
2. Numbness or Tingling You Can’t Ignore
A tingling or “pins-and-needles” sensation is one of the most common signs of nerve compression. This happens because the herniated disc is pressing on a nerve that carries signals between your spinal cord and the rest of your body. If ignored, these sensations can progress and affect balance or coordination, making early recognition crucial.
You might notice:
- Fingers are going numb while typing
- Tingling down your leg when walking
- Areas of reduced sensation that don’t improve with stretching
3. Weakness in Muscles or Grip
When nerves are compressed, they can no longer fully power the muscles they control. People with a herniated disc may find themselves:
- Dropping objects unexpectedly
- Stumbling while walking
- Struggling to lift your toes or perform basic movements.
Even small decreases in strength are a red flag and should not be mistaken for fatigue from a long day at work.
4. Pain That Changes With Posture
Unlike muscle soreness that improves with rest, herniated disc pain often intensifies in specific positions.
- Sitting for long periods can aggravate the pain
- Bending forward may make it sharper
- Standing or walking may temporarily relieve discomfort
5. Localized Back or Neck Pain That Persists
One of the earliest signs of a herniated disc can be a deep, gnawing ache in your lower back or neck. Unlike ordinary muscle soreness that improves with a day or two of rest, this pain lingers beyond 48 hours and may even gradually worsen.
You might notice it feels different from typical strain: it’s dull yet persistent, sometimes radiating slightly but mostly concentrated where the disc is affected. Paying attention to this kind of ongoing discomfort is important because it often precedes nerve-related symptoms
How Is a Herniated Disc Diagnosed by Doctors?
Diagnosing a herniated disc is a step-by-step process that helps doctors determine the precise source of your pain and the most effective treatment approach
1. Initial Assessment
It starts with a detailed medical history. Doctors ask about when the pain began, where it’s located, what triggers it (like bending, lifting, or sneezing), and any associated symptoms such as numbness, tingling, or weakness. A physical and neurological exam follows, checking reflexes, muscle strength, sensation, and specific movements like the straight-leg raise, to see if nerves are being irritated.
2. Imaging Tests
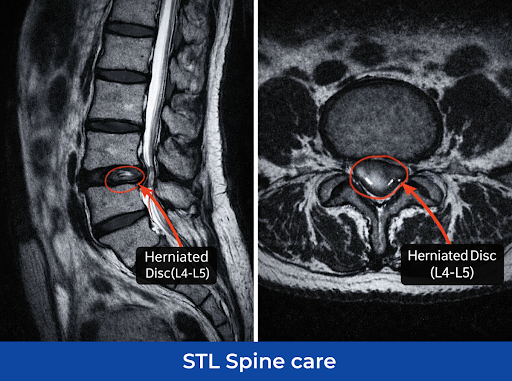
X-rays can rule out other issues like fractures, but do not show disc structures clearly. An MRI is the gold standard, allowing doctors to see the disc, nerves, and surrounding soft tissue. If an MRI isn’t possible, knowing whether CT scans or myelograms (X-rays with contrast dye) provide detailed spinal images and can reveal areas of nerve compression.
3. Advanced Tests
For a case situation where the person’s symptoms aren’t clear, electromyography (EMG) and nerve conduction studies (NCS) measure electrical activity in muscles and nerves to pinpoint nerve damage or compression. These tests are especially helpful when arm or leg symptoms overlap with other conditions.
Conclusion
Even mild back or neck discomfort can signal something more serious, like a herniated disc. Recognizing symptoms such as persistent localized pain, tingling, or weakness allows you to take action early. Understanding how your pain behaves and knowing the difference between a bulging and herniated disc puts you in control of your spine health.
If you’re wondering whether your herniated disc symptoms might improve on their own or risk getting worse without intervention, our detailed guide on Will a Herniated Disc Heal on Its Own or Get Worse Over Time? walks you through the body’s natural healing process and what to watch for.
STL Spine Care offers expert diagnosis and personalized treatment options, ensuring your spine stays healthy and functional. If you’re noticing these warning signs, acting now can make all the difference in your recovery and long-term spine health.
Frequently Asked Questions
What is a herniated disc, and how does it happen?
How do I know if my back pain is from a herniated disc?
Look for patterns such as pain radiating down your leg or arm, persistent localized discomfort, numbness or tingling, muscle weakness, or pain that changes with posture. These signs suggest nerve involvement rather than simple muscle strain.
What does a herniated disc feel like?
A herniated disc can feel like a deep, stubborn ache that suddenly turns into a streak of pain moving down your arm or leg. You may notice unusual sensations like buzzing, crawling, or partial numbness in certain areas.
When should I see a spine specialist?
Seek a specialist if you notice persistent pain, radiating symptoms, numbness, tingling, or muscle weakness. Urgent consultation is needed for severe weakness or loss of bladder/bowel control. STL SpineCare can provide expert evaluation and personalized treatment plans.
Are herniated discs more common in certain age groups?
Yes, adults between 30 and 50 years old are most commonly affected due to natural disc degeneration and wear-and-tear over time. Lifestyle factors like prolonged sitting or heavy lifting can increase risk.
